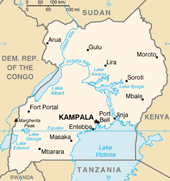
A country of 36 million, Uganda has the second highest fertility rate in the world. Despite progress over the last decade, maternal mortality remains high. Limited access to quality maternal care continues to put Ugandan women at risk of pregnancy-related disability as well. Obstetric fistula, a vaginal injury usually caused from prolonged labor without timely medical attention, is common, and many women are unaware that it can be treated and often repaired.
Since 2004, the Fistula Care project has worked with Ugandan health centers and hospitals to build awareness of obstetric fistula and support its prevention, treatment, and repair. Under the previous Fistula Care project from 2004 to 2013, we trained 26 doctors and 761 nurses to perform fistula repair surgery, and supported a total of 3,534 surgeries. We also greatly improved the quality of obstetric care and family planning services, both of which enable fistula prevention and worked with the ministry to help create “Learn From My Story,” a DVD of women with fistula sharing their stories. This collection is used in a variety of ways to raise awareness about the problem of fistula, both locally and worldwide.
Our work today continues to focus on strengthening fistula prevention and treatment in Uganda through the Fistula Care Plus project by expanding efforts to build community awareness, increasing emphasis on the integration of family planning services with fistula and maternal health care, and addressing the enormous backlog of women awaiting life-altering fistula repair.
In addition to thirteen prevention-only sites, Fistula Care Plus worked with three private, faith-based hospitals and two government-run referral hospitals to prevent and repair fistula:
- Hoima Hospital
- Kitovu Mission Hospital, Masaka District
- Kagando Mission Hospital, Kasese District
- Kamuli Mission Hospital
- Jinja Hospital
Supported Sites
Hoima Hospital is a regional referral hospital in western Uganda approximately 140 miles west of Kampala. The 280 bed public hospital offers a wide variety of services including a 29 bed maternity ward and an obstetric operating theater where fistula repair occurs. Hoima Hospital opened in as a district hospital in 1930, but since 1994 the hospital has served as a regional referral hospital serving 5 districts of Hoima, Buliisa, Kibaale, Kiryandongo and Masindi with a population of approximately 2 million people. Hoima Hospital conducts fistula repair outreach, holds concentrated repair sessions, provides family planning services to fistula patients, and conducts refresher training courses. With support from Fistula Care, the health facility pioneered the implementation of the mentoring and coaching strategy for fistula surgeons in Uganda.
Kitovu Mission Hospital is located 120 km southwest of Kampala in Masaka District, on the shores of Lake Victoria. The 200-bed hospital has a special fistula repair clinic, which serves as a referral site for complex fistula repairs. Visiting master surgeons regularly hold camps at Kitovu Hospital at which many women with fistula can be repaired at once. This provides an important opportunity to train both new and existing fistula surgeons, along with surgical teams. Fistula Care is helping Masaka District Hospital, a 240-bed public hospital nearby, to refer patients with fistula to Kitovu Hospital and to strengthen its emergency obstetric care to prevent new fistulas from occurring.
Kagando Mission Hospital is located in Kasese District in southwestern Uganda, along the Congolese border. It opened in 1965 as a hospital primarily for lepers operated by the Africa Inland Mission. Over time, the Kagando Hospital diversified greatly, and today it offers 200 beds and services ranging from maternity to surgery to health education. The hospital is part of a rural development initiative that focuses on prevention, invites voluntary service, and encourages the community to be part of the decision-making process. Fistula Care is working with Bwera District Hospital, a public hospital with 120 beds, to refer fistula patients to Kagando Hospital and to improve its emergency obstetric services.
Kamuli Mission Hospital is a private, non-profit, community hospital owned by the Roman Catholic Diocese of Jinja and is accredited by the Uganda Catholic Medical Bureau. The hospital is administered by the Little Sisters of St. Francis. The planned bed-capacity of the hospital is 160.
Jinja Hospital is a regional referral hospital in the city of Jinja, eastern Uganda. It is the largest hospital in eastern Uganda, with a bed capacity of 600. Jinja Hospital is one of the thirteen regional referral hospitals in Uganda and one of the fifteen (15) hospitals designated as internship hospitals, where graduates of Ugandan medical schools may undergo a year of internship under the supervision of consultants and specialists, including surgical specialties.
Uganda Resources
Five Years of Fistula Care Plus: Looking Back at Key Achievements and the Way Forward to End Fistula (English and French PDF, 2476 KB) EngenderHealth. Fistula Care Plus (FC+) is a global project initiated in 2013 by the US Agency for International Development (USAID) and implemented by EngenderHealth. FC+ builds on and enhances the work undertaken by USAID’s previous Fistula Care project (2007–2013), also led by EngenderHealth. Achievements from the first five years of project implementation (December 2013–December 2018) in Bangladesh, DRC, Mozambique, Niger, Nigeria, Togo, and Uganda are summarized in this brief.
Use of interactive voice response technology to address barriers to fistula care in Nigeria and Uganda. (Fistula Care Plus and Population Council, 2020). The use of digital health technologies has expanded across low-resource settings, including in programs seeking to improve maternal health care seeking and service usage. However, there has been limited use of these technologies for screening and referral within maternal health, and many interventions have relied on SMS tools, which may have limited impact in settings with low female literacy. Digital health technologies have the potential to increase access to care for chronic maternal morbidities, such as obstetric fistula, and for women facing stigma, geographic isolation, and other sociocultural barriers to care seeking. This study documented the process of developing and implementing an innovative fistula screening and referral hotline using interactive voice response (IVR) technology, and described the service usage results and stakeholder perspectives associated with the hotline.
Fistula Care Plus in Uganda: Success Stories (English, PDF, 3439 KB), EngenderHealth. A compilation of success stories from clients, clinicians, and others involved with the Fistula Care Plus project in Uganda.
Improving Quality of Life for Women with Incurable Fistula: A Fistula Care Plus and TERREWODE Research Partnership in Uganda (English, PDF, 1300 KB) EngenderHealth and TERREWODE. EngenderHealth’s Fistula Care Plus (FC+) project
partnered with a Ugandan organization, the Association for the Rehabilitation and Re-orientation of Women for
Development (TERREWODE), to conduct research on the social reintegration needs of these women and evaluate
the effects of interventions responding to these needs.
Communities and Health Workers Improving Maternal Health Together in Jinja District, Uganda (English PDF 1658 KB, French PDF 1711 KB) EngenderHealth, 2019. In June 2016, Fistula Care Plus introduced the site walk-through (SWT) model in Jinja, Uganda. An SWT is a one-day event that aims to gather the views of community representatives and health providers on challenges and opportunities for increasing access to services at the health facility in order to inform strategies for strengthening linkages between the health facility and the catchment population. The experience of utilizing the SWT model within FC+ Uganda is highlighted in this brief.
Engaging Religious Leaders in Support of Maternal Health in Uganda (English PDF, 1858 KB, French PDF, 1.68 MB) EngenderHealth, 2019. To increase awareness, the FC+ project leveraged existing communication strengths by engaging religious leaders and fostering their support for maternal health and family planning services. This brief documents the FC+ program experience, focusing on the religious leaders’ perspectives and key lessons learned.
Empowering Youth through Social and Financial Life Skills and Healthy Behaviors: Lessons from a Ugandan Pilot (English PDF 1386 KB, French PDF 1370 KB) EngenderHealth, 2019. FC+’s Aflateen PLUS youth engagement strategy paired an integrated curriculum with dual strategies for in- and out-of school youth. This approach could be replicated in Uganda and other low-resource settings to support youth in developing life skills and planning a healthy future.
Development and preliminary validation of a post-fistula repair reintegration instrument among Ugandan women. Reproductive Health. 2017 Sep 2;14(1):109. FC+ supported research teams from UCSF’s Bixby Center for Global Reproductive Health and Makerere University to conduct an exploratory sequential mixed-methods study with women who underwent fistula surgery within two previous years to inform measure development and validate a measurement instrument.
Improving Partograph Use in Uganda through Coaching and Mentoring (English, PDF, 1.82 MB; French, PDF, 1.4 MB) EngenderHealth, August 2013
Since 2010, Fistula Care has collaborated with the Reproductive Health Department of the Ugandan Ministry of Health to strengthen partograph use. This technical brief describes the challenges and achievements of developing and implementing a new approach to support partograph use in five facilities across three districts and makes recommendations for future partograph programming at the national, district, and facility levels.
Creating an Enabling Environment for Fistula Prevention and Treatment in Uganda (English, PDF, 14 KB; French, PDF, 2.1 MB) EngenderHealth, March 2013
The Fistula Technical Working Group was established by the Ugandan Ministry of Health’s Clinical Services Department to ensure equitable access to health care for women with fistula, promote prevention strategies, maximize the efficient use of resources, eliminate duplication of effort, and foster a community of providers. This brief describes three important achievements of the Uganda Ministry of Health and the Fistula Technical Working Group: building an information base for obstetric fistula to better plan for and manage prevention, treatment, and reintegration services; integrating fistula services into the Uganda health system; and establishing standards, guidelines, and protocols to guide services.
For more learnings from Uganda and other FC+ countries, visit our Resources section.