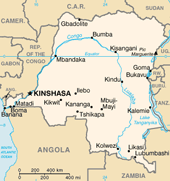
 The Democratic Republic of the Congo (DRC) borders nine countries in central Africa and is approximately the size of the United States east of the Mississippi. After nearly four decades of war and conflict, people living in the DRC face numerous barriers to accessing quality reproductive health services. Due to its vast size and poorly developed road and communication systems, family planning and other basic services are extremely limited or altogether unavailable. Poor maternal health care has resulted in high maternal mortality as well as the occurrence of obstetric fistula, often caused by obstructed labor. Traumatic fistula—the same condition inflicted by sexual violence—is also common, due to the prevalence of gender-based violence in the DRC.
The Democratic Republic of the Congo (DRC) borders nine countries in central Africa and is approximately the size of the United States east of the Mississippi. After nearly four decades of war and conflict, people living in the DRC face numerous barriers to accessing quality reproductive health services. Due to its vast size and poorly developed road and communication systems, family planning and other basic services are extremely limited or altogether unavailable. Poor maternal health care has resulted in high maternal mortality as well as the occurrence of obstetric fistula, often caused by obstructed labor. Traumatic fistula—the same condition inflicted by sexual violence—is also common, due to the prevalence of gender-based violence in the DRC.
Since 2008, Fistula Care has worked to improve the quality of and access to fistula care services in the DRC. Under the original Fistula Care project from 2008 to 2013, we partnered with seven health centers and hospitals to train 44 doctors and 242 nurses in fistula repair surgery and 802 doctors and nurses in fistula counseling and follow-up care. Our work also included the improvement of emergency obstetric care and outreach to rural clinics to ensure that women in need of medical attention were referred to the hospitals for repair.

EngenderHealth continued the work in DRC through Fistula Care Plus, specifically addressing the backlog of women living with obstetric or traumatic fistula. We are also increasing the integration of family planning services with fistula and maternal health services as a key component of fistula prevention.
FC+ directly supported six health facilities for fistula treatment and prevention services, including private and faith-based health facilities in five provinces: Kinshasa, Lubumbashi, Maniema, North Kivu, and South Kivu. Through these partnerships, FC+ supported fistula repairs and worked to prevent fistula by supporting voluntary family planning (FP), clinical capacity building, and community outreach and education. The project emphasized strengthening systems for safe surgery (including routine fistula repair), community awareness, FP services integration with fistula and maternal health care, and reintegration of women who have undergone fistula repair. The project also supported FP and fistula prevention services at an additional 318 facilities in Ituri and North Kivu provinces.
- HEAL Africa Hospital, Goma, North Kivu
- Imagerie des Grands Lacs, Beni, North Kivu
- Kisenso Hospital, Kinshasa
- Maternité Sans Risque de Kindu, Kindu, Maniema
- St. Joseph Hospital, Kinshasa
- The General Referral Hospital of Panzi, Bukavu, South Kivu
Supported Sites
HEAL Africa Hospital is a faith-based hospital in the North Kivu capital, Goma. HEAL Africa began as a small surgical training clinic in 1996, and over time it has expanded its services to become a 180-bed hospital that performs more than 280 fistula surgeries per year. Local volunteers help to identify patients and bring them to the hospital. At any given time, between 120 and 160 women are waiting for fistula repair at the hospital. HEAL Africa also works with village and religious leaders to develop plans to care for the area’s vulnerable populations.
Imagerie des Grands Lacs is a private, non-profit facility located in the remote city of Beni in North Kivu province. The facility has 10 beds dedicated to fistula patients and serves a catchment population of 1.5 million, most of who are dispersed throughout the surrounding rural area, where demand for fistula repair services is extremely high. The hospital has one fistula surgeon and receives funding from Fistula Care to provide 108 fistula repairs each year.
Kisenso Hospital is a secondary referral hospital in Kinshasa, and like St. Joseph’s Hospital, is also managed by the Archdiocese. At this time, fistula repair services are not available because the hospital does not have trained fistula surgeons. The hospital provides emergency obstetric services around the clock and the resident surgeon and support staff participate in exercises conducted by Fistula Care in Kinshasa with the goal of training the resident surgeon to provide fistula repair.
Maternité Sans Risque de Kindu (MSRK) is a private, non-profit hospital located in Kindu, Maniema province, in the remote interior of the DRC. MSRK has 31 beds and performs routine fistula surgeries three days a week. In addition to supporting the cost of fistula repair surgery, Fistula Care also provides opportunities for quality improvement and infection prevention training to MSRK staff, and provides equipment critical to successful fistula repair. MSRK is one of the only fistula repair centers in Maniema Province, and the facility is an important regional resource for women suffering from obstetric fistula.
St. Joseph Hospital is a private, faith-based hospital located in Kinshasa, the capital of the Democratic Republic of Congo. St. Joseph’s was originally constructed as a convent by the Bureau Diocesien des Oeuvres Medicales (the Archdiocese for Medical Services) but converted into a hospital in 1987, with fistula repair services beginning in 2003. The hospital, a tertiary referral center, serves a catchment area of 2 million people. The hospital also treats difficult cases from outside of its catchment area. Fistula Care supports fistula repairs at St. Joseph’s Hospital, in addition to building the capacity of its resident fistula surgeon through surgical training exercises.
The General Referral Hospital of Panzi is located in Bukavu, the capital of South Kivu. It opened in 1999, and in spite of numerous setbacks during the wars, it has grown to a 334-bed faith-based hospital that offers a diverse array of medical and surgical services. More than 70% of Panzi patients are survivors of sexual violence. Given the facility’s expertise in repairing fistula, patients now come to Panzi from all over the Kivu provinces in Eastern Congo and beyond.
At a Glance: FC+ DRC
• 3,364 surgical fistula repairs completed; 95% closed at discharge
• 7 fistula surgeons and 5,175 other healthcare workers trained in fistula prevention and treatment
• 93,262 family planning counseling sessions and 79,424 couple-years of protection delivered at project-supported health facilities
• 34,042 individuals reached through in-person community outreach
DRC Resources
Fistula Care Plus: Democratic Republic of Congo (DRC)- Strengthening Health Systems to Prevent and Treat Fistula (English PDF, French PDF) USAID-supported fistula prevention and repair efforts in the Democratic Republic of Congo (DRC) began in 2005 and continued under the Fistula Care and FC+ projects, until March 2021. Fistula is a devastating morbidity, with profound social consequences for those affected. In the DRC, FC+ directly supported six health facilities for fistula treatment and prevention services, including private and faith-based health facilities in five provinces: Kinshasa, Lubumbashi, Maniema, North Kivu, and South Kivu. Through these partnerships, FC+ supported fistula repairs and worked to prevent fistula by supporting voluntary family planning (FP), clinical capacity building, and community outreach and education. The project emphasized strengthening systems for safe surgery (including routine fistula repair), community awareness, FP services integration with fistula and maternal health care, and reintegration of women who have undergone fistula repair. The project also supported FP and fistula prevention services at an additional 318 facilities in Ituri and North Kivu provinces.
FC+ End of Project Report Summary Operating in seven countries—Bangladesh (2013-2020), the Democratic Republic of Congo (DRC: 2014 -2021), Mozambique (2017-2021), Niger (2013-2021), Nigeria (2014-2018), Togo (2014), and Uganda (2014-2019) — FC+ focused on five objectives:
1. Strengthening the enabling environment to institutionalize fistula services in the public and private sectors.
2. Enhancing community understanding and practices to prevent fistula, improve access to treatment, reduce stigma and
support reintegration.
3. Reducing transportation, communications, and financial barriers to care.
4. Strengthening provider and health facility capacity to provide and sustain quality services.
5. Strengthening the evidence base to improve fistula care and scale up application of standard M&E indicators for prevention and treatment.
Fistula Care Plus: Key Achievements and the Way Forward to End Fistula (English PDF, French PDF) Fistula Care Plus (FC+) was a global project initiated by the United States Agency for International Development (USAID) and implemented by EngenderHealth from December 2013 to March 2021. Building on work undertaken by the previous Fistula Care project (2007 to 2013), FC+ supported activities in 1,171 facilities (54 fistula treatment sites and prevention sites and 1,117 prevention-only sites) in Bangladesh, Democratic Republic of Congo (DRC), Mozambique, Niger, Nigeria, Togo, and Uganda. The data presented in this brief covers these time periods
Fistula Care Plus: Summary of Repair Case Profiles and Outcomes FC+ collected routine client data on surgical and nonsurgical fistula repairs at all project-supported fistula treatment sites through 1.) aggregate facility data, reported on a quarterly basis by treatment sites and entered into a project-developed DHIS2 platform for data storage and analysis and 2.) individual client data collected at a subset of 27 project-supported facilities in four countries. Through these mechanisms, FC+ and project-supported facilities were able to routinely monitor and act upon identified clinical trends at the facility, country, and global levels. This brief summarizes routine, aggregated, and anonymous global and country project data on demand for and provision of fistula repair services and illustrates client profiles including the causes of clients’ fistula, fistula types, surgical outcomes, and family planning (FP) preferences and uptake.
Frequency and management of non-obstetric fistula in the Democratic Republic of Congo: Experience from the Fistula Care Plus project. Trop Med Int Health, June 2020. In order to describe the frequency, causes and post‐repair outcomes of non-obstetric fistula (NOF) in hospitals supported by the Fistula Care Plus (FC+) project in the Democratic Republic of Congo, FC+ staff and partners conducted a retrospective cohort study from 1 January 2015 to 31 December 2017 in three FC + supported fistula repair sites. Of 1984 women treated for female genital fistula between 2015 and 2017 in the three FC + supported hospitals, 384 (19%) were considered to be NOF cases.
Five Years of Fistula Care Plus: Looking Back at Key Achievements and the Way Forward to End Fistula (English and French PDF, 2476 KB) EngenderHealth. Fistula Care Plus (FC+) is a global project initiated in 2013 by the US Agency for International Development (USAID) and implemented by EngenderHealth. FC+ builds on and enhances the work undertaken by USAID’s previous Fistula Care project (2007–2013), also led by EngenderHealth. Achievements from the first five years of project implementation (December 2013–December 2018) in Bangladesh, DRC, Mozambique, Niger, Nigeria, Togo, and Uganda are summarized in this brief.
What to measure and why? Experience developing monitoring indicators for an emerging maternal health issue: the case of obstetric fistula. Journal of Health Informatics in Developing Countries, 2015.
Carrie Ngongo, Evelyn Landry, Karen Levin, Simon Ndizeye, Iretioluwa Sutton, and Vandana Tripathi recounts the process of developing, refining, and using standardized monitoring indicators as part of a fistula prevention and repair project in fourteen countries—Bangladesh, Benin, Democratic Republic of the Congo, Ethiopia, Ghana, Guinea, Liberia, Mali, Niger, Nigeria, Rwanda, Sierra Leone, Togo, and Uganda.
Living with Obstetric Fistula: Qualitative Research Findings from Bangladesh and the Democratic Republic of the Congo (English, PDF, 1 MB; French, PDF, 750 KB) EngenderHealth, August 2012
What are the social consequences of fistula? What affects how women with fistula are treated? Fistula Care is pleased to announce its latest technical brief, which provides insights into the experiences of women with fistula in Bangladesh and the Democratic Republic of the Congo. This qualitative research examines the lives of women suffering from fistula in two very different sociocultural contexts, including the physical and social consequences associated with the condition and women’s attempts to obtain care.
Fistula and Traumatic Genital Injury from Sexual Violence in a Conflict Setting in Eastern Congo: Case Studies Reproductive Health Matters, May 2008, Volume 16, Issue 31.
Ahuka Ona Longombe, Kasereka Masumbuko Claude, and Joseph Ruminjo document stories from sexual violence survivors in the Democratic Republic of the Congo.
For more learnings from the Democratic Republic of Congo and other FC+ countries, visit our Resources section.


